 One of the foundation stones for the so-called “sexual revolution” of the 1960s was set in place 57 years ago today, with the announcement that “the pill” would be available on the NHS.
One of the foundation stones for the so-called “sexual revolution” of the 1960s was set in place 57 years ago today, with the announcement that “the pill” would be available on the NHS.
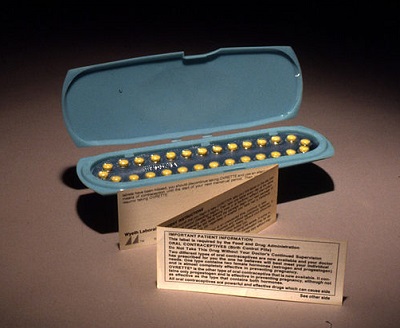
Before then it was only prescribed in a small number of cases on purely medical grounds, but on December 4th, 1961, it was announced that oral contraception – widely known as “the pill” – would be available on the NHS for women who requested it.
 The announcement was made in the House of Commons by Health Minister Enoch Powell, but he didn’t give any specific guidance about who should or shouldn’t get the pill, saying that was a matter for doctors.
The announcement was made in the House of Commons by Health Minister Enoch Powell, but he didn’t give any specific guidance about who should or shouldn’t get the pill, saying that was a matter for doctors.
Some GPs complained that left doubt over whether they could prescribe the oral contraceptive for ‘social’ as well as medical reasons – in other words, to women who simply didn’t want to get pregnant as well as to those for whom pregnancy was medically inadvisable. Such confusion evaporated as more and more women visited their GPs asking to go ‘on the pill’ and doctors who prescribed it soon discovered they were free to do so without reprimand.
For other politicians, the bigger concern was the cost to the economy. The NHS was already spending £90 million per year on its drugs bill, and that was set to increase significantly if there was a high demand for the oral contraceptive, which had to be taken every day in order to be effective.
‘The pill’ was a combination of synthetic hormones oestrogen and progestogen which together altered a woman’s menstrual cycle to prevent ovulation and pregnancy. Although it had been extensively tested and was already widely available in the USA, some doctors had concerns over its long-term effects on women who chose to use it.
Sir Charles Dodds, at that time Britain’s leading expert on the drugs used in the pill, warned it could have long-term side-effects and should only be used after careful consideration of all the alternatives. He compared a woman’s body to the workings of a clock, saying: “Even if you thoroughly understand the mechanism of a clock, provided it is going well it is very much better to leave it alone. To interfere with it if you do not understand it can be disastrous.”
There were also hotly-debated moral questions about who should or shouldn’t get the pill. Some ethical and religious campaigners said it should be banned outright, while others said it should only be available to married women, as unmarried women should not be having sex anyway. Some also said that married women should only be allowed it with their husband’s express permission.
The Family Planning Association, which ran clinics throughout Britain, was still deciding whether its physicians should offer the pill to married women who requested it. In practical terms it was usually left to individual doctors to decide which of their patients, married or single, should be prescribed the pill if they asked for it. Doctors who refused it soon found that patients were free to register with another doctor who might be more sympathetic to their request.
Opponents of the pill said it gave women licence to be promiscuous without fear of the likely consequences. Supporters countered that it gave women a new sexual freedom of choice never before enjoyed by their gender. Within a few years it was in widespread use and, in most cases, available to any woman over 16 who requested it from their GP. It proved an extremely effective method of birth control and although some women experienced limited side-effects, they became less common as new versions of the pill were developed.
In 2003 scientists announced they had developed a male version of the pill – a hormonal contraceptive which worked through an implant under the skin combined with an injection every three months. There was no need to take a pill every day and the treatment was free of side-effects, but somehow it hasn’t caught on. Today it is estimated that a third of UK women aged 16 to 49 currently use the contraceptive pill, which is by far the most popular form of reversible contraceptive and is 99.7% effective.
