ANYONE awaiting surgery in a hospital operating theatre can be forgiven for feeling a little anxious – surgery will always carry a calculated risk, but it is now safer than it has ever been.
One of the main reasons for that is a simple but highly effective checklist for surgical teams, which has saved countless lives and improved patient outcomes not just in the UK but around the world.
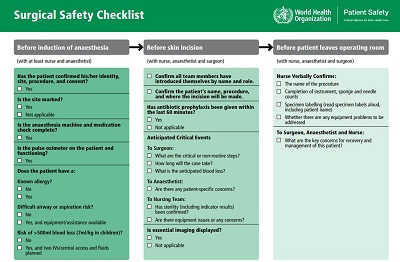 It is now 10 years since the standardised checklist was launched by the World Health Organisation (WHO). It was created with substantial input from UK clinicians and mandated for use throughout the NHS in 2009. In the decade since, a wide range of studies and evaluations have consistently shown the checklist to reduce the rate of deaths and surgical complications by as much as one-third in facilities where it is used.
It is now 10 years since the standardised checklist was launched by the World Health Organisation (WHO). It was created with substantial input from UK clinicians and mandated for use throughout the NHS in 2009. In the decade since, a wide range of studies and evaluations have consistently shown the checklist to reduce the rate of deaths and surgical complications by as much as one-third in facilities where it is used.
The operating theatre is the most common site for adverse surgical incidents, with errors occurring in nearly 15% of all patients globally, and some international studies suggesting that surgery may be responsible for up to a million deaths every year and up to seven million post-operative complications.
Thanks to funding provided by the UK during its EU Presidency in 2005, and with extensive involvement of UK clinicians, the WHO started work to address this in 2006, producing the first ever global guidelines for safe surgery. These guidelines were then developed into the ‘Surgical Safety Checklist’, modelled on the pre-flight checklist which pilots undertake.
The checklist is a simple tool designed to improve communication and teamwork by bringing together the surgeons, anaesthesia providers and nurses involved in care to confirm that critical safety measures are performed before, during and after an operation. Development of the checklist was led by Pauline Philip, who was then Director for Patient Safety at the WHO. Today she is National Director for Emergency and Elective Care for the NHS in England and continues to help promote surgical safety around the world.
She said: “The safety of patients should always be the number one priority for the NHS, and for any health system around the world. It was a privilege to work with some of the country’s leading clinicians to develop this checklist to support safety in operating theatres around the world, and a source of pride that the NHS led the world in piloting and adopting it.”
Early pilots in eight hospitals found that using the checklist reduced the rate of deaths and surgical complications by more than one-third across all eight sites. The rate of major inpatient complications dropped from 11% to 7%, and the inpatient death rate following major operations fell by almost half from 1.5% to 0.8%.
Working through the 19-items on the checklist for any surgical procedure addresses serious and avoidable surgical complications, by ensuring that critical steps outlined in the guidelines are done in every surgery, every time, everywhere. It also serves as a critical communication tool for the operating theatre team, who might be working together for the first time, or might have worked together many times before, which risks complacency.
Professor Derek Alderson, President of the Royal College of Surgeons said: “The WHO surgical safety checklist has demonstrated that even simple innovations can have profound patient safety benefits in healthcare. Since its introduction, countless harmful incidents have been avoided and it has helped to create a safety-first culture in the NHS. There is no excuse for surgical teams not to use it.
“Over the next decade it will be vital to help spread its adoption in other parts of the world. Once again, surgery in the NHS will act as a global role model.”
The checklist has now been adopted in a range of countries around the world. Its success has also led to the development and introduction of similar checklists in a range of other clinical areas, including childbirth, emergency departments, and intensive care units.
